Themes > Features
29.11.2011
Why are Women’s Health Outcomes in India so Poor?*
There
are several senses in which the health of women and girls can be considered
as the basic indicators for the health of a society. Precisely because
of gender discrimination, the health conditions of females generally
tend to lag behind those of males, and therefore absolute improvement
in these conditions is a reasonable indicator that the overall health
conditions of that society are also getting better.
In the past two decades, India had the third fastest growing economy
in the Asian region (after China and Vietnam) and it is generally perceived
even in a period of continuing global crisis, as an emerging economic
powerhouse. Table 1 presents India’s growth performance in the past
two decades in relation to three other Asian countries. Vietnam grew
slightly faster than India but still has slightly lower per capita income.
Sri Lanka is richer on average but has growth more slowly, while Bangladesh
is still clearly a low income country, where per capita income has increased,
though more slowly than these other countries.
Table
1: |
||||
Annual
per capita income change 1990-2010 (%) |
National
Income per capita, US $ in 2010
|
|||
Bangladesh |
3.49 |
700
|
||
India |
4.90 |
1340
|
||
Sri
Lanka |
4.22 |
2240
|
||
Vietnam |
5.95 |
1110
|
||
To what extent was this period of economic expansion in India reflected in better health outcomes for women and girls? To examine this, we consider two crucial health indicators: the female Infant Mortality Rate (IMR or number of deaths per 1000 children below one year) and the Maternal Mortality Ratio (MMR or number of childbirth-related deaths per 100,000 live births).
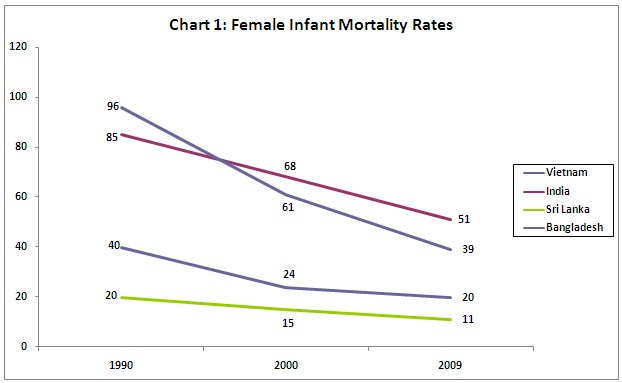
Chart 1 shows that in terms of female infant mortality rates, India is by far the worst performer in this group, with the slowest rate of decline. Even Bangladesh, which is much poorer and has slower national income growth, managed to bring the female IMR down faster. And the Indian rate is more than two and a half times that of Vietnam, which has a lower per capita income.
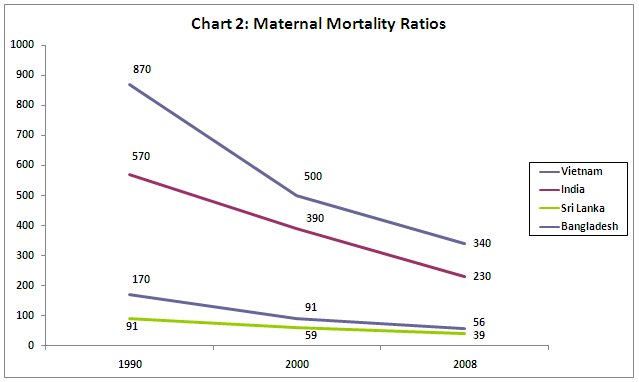
The evidence on maternal mortality is equally disturbing. India and
Bangladesh both have very high rates, many multiples of those in Sri
Lanka and Vietnam. But even here, the rate of reduction of this ratio
has been marginally faster in Bangladesh.
Of course India is also very regionally diverse, with some states like
Kerala showing excellent health outcomes for women, similar to those
in Vietnam. And three states have also shown much improved health indicators
in the past two decades: Tamil Nadu, West Bengal and Maharashtra. But
the bulk of the country still shows generally appalling levels of female
IMR and MMR.
One important reason for high infant and child mortality is under-nutrition,
which has actually worsened in recent times according to indicators
like calorie consumption. Rising prices of food are making this problem
worse as women and girls in poor households take the brunt of food scarcity.
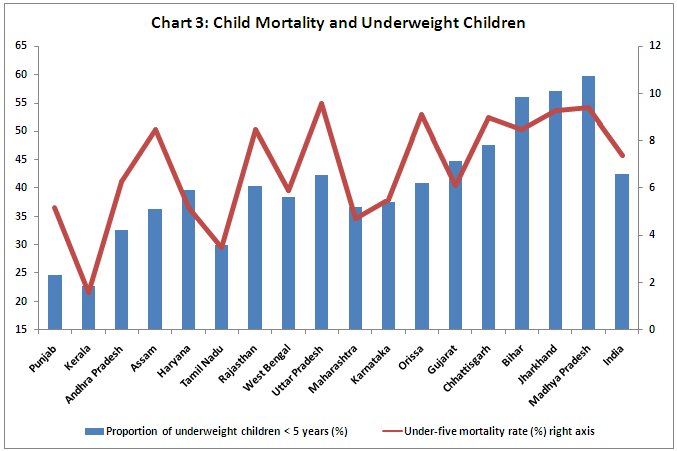
Chart 3 shows how closely the rate of child mortality tracks the proportion
of underweight children across Indian states.
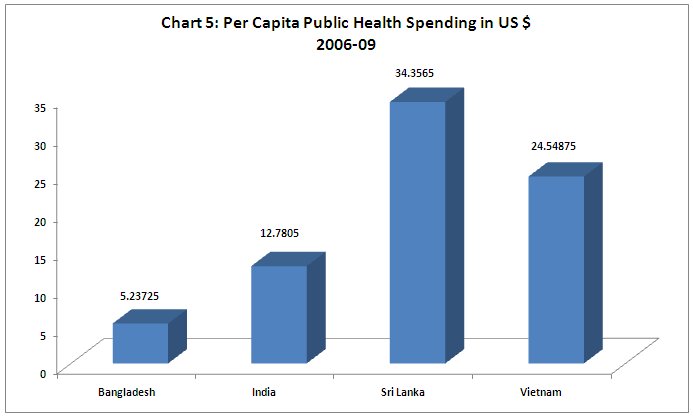
Nutrition is important, but it is not the only concern. To deliver better health outcomes, public expenditure on health service delivery is absolutely essential, and this is especially important for women and girl children. Here again, India fares badly. Public spending on health (as Chart 4 shows) is a minuscule amount in relation to GDP, and around two-third of health expenditure is out-of-pocket payment by households. This is indeed an important reason for families falling into poverty or remaining destitute, and gender biases reinforce the relative denial of health care to women and girls in such conditions.
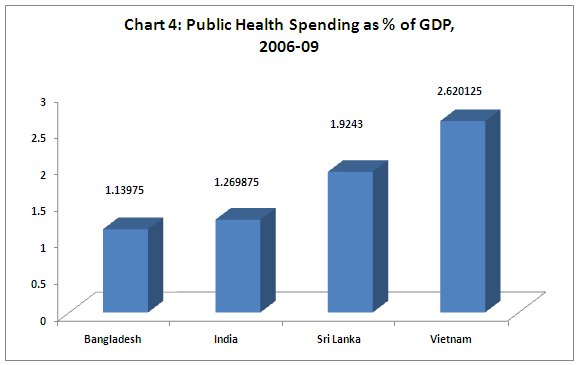
Even in absolute per capita terms, public health spending in India is around half that in Vietnam, which is a country with lower per capita income. And it is just above one-third of the level in Sri Lanka. It is true that Bangladesh show a much lower level, but then Bangladesh also has a much lower per capita income.
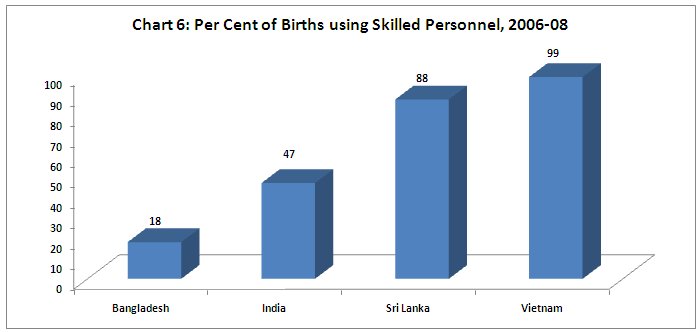
So it is no wonder that other indicators of health service delivery also appear quite inadequate with respect to the other countries. Chart 6 shows that less than half of births are attended by skilled personnel, whereas in Vietnam it is near universal and it is close to that in Sri Lanka. The low proportion here suggests one important reason for the high maternal mortality ratios in India and Bangladesh.
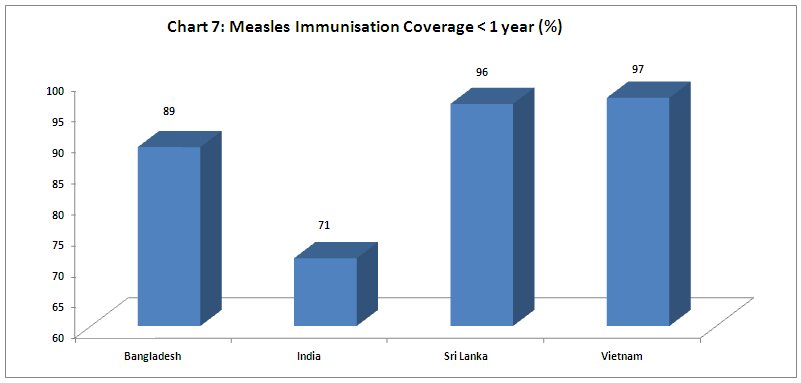
Similarly, immunisation coverage is a necessary element in ensuring child health. Full measles coverage within the first year of life is often taken as a proxy for the extent of immunisation in general, and in this case India fares worst among this set of four countries. Even Bangladesh has much higher immunisation rates. In some parts of the country, immunisation rates have barely improved. Small wonder then, that infant mortality rates has come down more slowly in India than in these other countries.
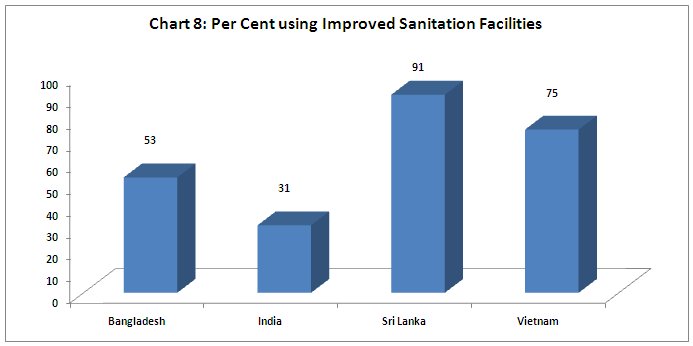
Another major aspect of ensuring adequate health conditions is the provision of improved sanitation for everyone. This is one of the weakest aspects, along with nutrition: around 70 per cent of the population do not have access to improved toilets. Remarkably, this does not even appear as a major policy goal for the government, which does not appear to see the urgency in this matter, or the wider health effects, quite apart from the loss of dignity to citizens that comes from forced open defaecation.
All
of these factors are crucially determined by government policy. Despite
much publicly expressed concern on all these issues, the Government
of India has simply not put its money where its mouth is. Public spending
as a share of GDP has not increased, and per capita spending on some
essential activities like immunisation and primary health centres has
actually gone down. Instead, the government has sought to provide essential
health services on the cheap, using the underpaid labour of local women
working for much less than the minimum wage, not properly trained regular
public employees with adequate facilities.
The apparently growing divide between economic growth and women’s health
outcomes in countries like India is not inevitable: the experience of
other Asian countries shows that a more positive synergy can be created,
with health spending not just valued for its own sake, but as an essential
element in an overall macroeconomic and growth framework oriented to
better conditions of human life rather than just GDP expansion.
*
This article was originally published in the Business Line on November
28, 2011.
©
MACROSCAN 2011